Written by: Becca Malizia, MS, Bonnie Feldman, DDS, MBA, Ellen M. Martin
Alzheimer’s disease is a devastating neurodegenerative disease. Although not technically an autoimmune disease, it is considered an inflammatory disease and shares many connections with autoimmune diseases. The cause of Alzheimer’s is currently unknown and its etiology is not completely understood. New evidence is beginning to shed light on the connection between the oral microbiome and Alzheimer’s. This emerging information may also be important for other autoimmune and immune-related diseases — a link that may be able to put the puzzle pieces together…
To answer some of our questions surrounding the oral microbiome and Alzheimer’s disease, we interviewed Kacey Haptonstall, a graduate student in the Fox lab at UCLA, who is currently conducting research on this very topic!
Her research in a nutshell
Haptonstall and the Fox lab at UCLA work mostly on researching the inflammatory pathways that influence Alzheimer’s risk, how those pathways are, in turn, influenced by the oral microbiome, and how the oral microbiome has changed through history, resulting in an increased risk for Alzheimer’s in humans.
Why focus on the oral microbiome?
“The oral microbiome is an untapped market.”
 Coming from a more holistic background, it seemed crazy obvious to Haptonstall that the health of the mouth would be linked to Alzheimer’s disease, considering the mouth is an essential part of the head. The more digging she did, the more she found quite a lot of support linking the mouth to Alzheimer’s. Many people with Alzheimer’s also suffer from tooth loss and periodontal disease. But the story doesn’t stop there. A specific oral pathogenic microbe, P. gingivalis, already known for contributing to tooth loss and periodontal disease, has recently been implicated in Alzheimer’s. Stay tuned to learn more about the possible causational evidence for this oral microbe and Alzheimer’s disease, in our next article to be published soon.
Coming from a more holistic background, it seemed crazy obvious to Haptonstall that the health of the mouth would be linked to Alzheimer’s disease, considering the mouth is an essential part of the head. The more digging she did, the more she found quite a lot of support linking the mouth to Alzheimer’s. Many people with Alzheimer’s also suffer from tooth loss and periodontal disease. But the story doesn’t stop there. A specific oral pathogenic microbe, P. gingivalis, already known for contributing to tooth loss and periodontal disease, has recently been implicated in Alzheimer’s. Stay tuned to learn more about the possible causational evidence for this oral microbe and Alzheimer’s disease, in our next article to be published soon.
If this connection is so important, why have we just begun to look into the oral microbiome?
One of the biggest problems with our healthcare system is that while specialization has enabled us to dive deep into specific parts of the body and disease, it has left us trapped in silos, forgetting that the body is one interconnected system. Haptonstall explained that traditionally, Alzheimer’s has been thought of as only a brain problem, ignoring other parts of the body. Disease research often neglects a holistic approach, an avenue that is getting more traction recently (thankfully). Haptonstall believes that doctors and dentists should collaborate more, especially for a disease like Alzheimer’s that has such a deep connection to the mouth.

So why Alzheimer’s disease?
Like many others, the interest is a personal one. In 2013, Haptonstall explained that her near and dear grandmother was diagnosed with Alzheimer’s. “My mom quit her job and moved to go take care of my grandma. Watching my grandma degrade over time has been devastating. She was my idol, and to see what a disease can do to a living human without killing — it’s unbelievable.” As a result, she threw her dream of being a park ranger aside, opting for a mission to do this research and help people.
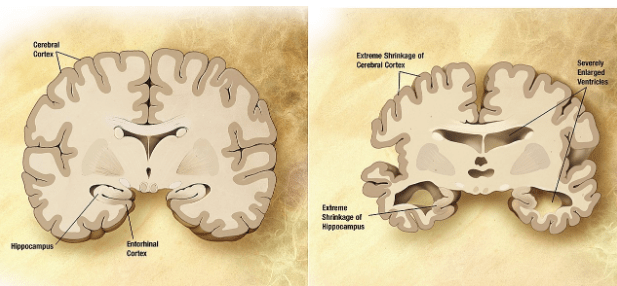
image source: wikicommons
What connections are being made between the oral microbiome and Alzheimer’s?
Haptonstall’s UCLA lab, lead by Molly Fox, PhD, believes in the transient bacteremia theory. This theory expands on the idea that when you floss, have a dental procedure, or disrupt the mucosal barrier in the mouth (think about getting a cut on your skin) oral bacteria can enter the bloodstream and subsequently get into the brain. Since the oral bacteria are not supposed to be anywhere but the mouth, this can cause an inflammatory response. The natural inflammatory reaction can cause a cascading and long-lasting inflammatory response, resulting in a buildup of amyloid plaques (one of the known hallmarks of Alzheimer’s). This is important to autoimmune diseases in general; in theory, this misplaced bacteria triggered inflammation, could happen not just in the brain, but all over the body.

Image source (1): cortexyme.com
Are the beta amyloid plaques all bad?
Beta amyloid plaques are a natural part of the innate immune response of healthy individuals. They have antimicrobial properties and are one of the first lines of defense against invading pathogens. The problem arises when they don’t get properly cleared. In a healthy individual, a pathogen comes in, beta amyloid plaques form, and then they go away. If they don’t go away, they build up and can cause prolonged and harmful inflammation. Haptonstall stated that this is linked to the infamous APOE4 allele, which seems to be particularly bad at clearing out the plaques.
Is this similar to the oral microbiome and other neurodegenerative and autoimmune diseases?
While her expertise lies in Alzheimer’s, Haptontall hypothesizes that this could be a problem in ANY disease where inflammation is a problem. Once the oral bacteria enter the bloodstream, it’s possible for them to travel anywhere in the body. If they don’t get properly cleared by the immune system, they could cause inflammation in any organ in the body. We believe that this could potentially be important in Multiple Sclerosis, Fibromyalgia, even cardiovascular disease.
Oral microbiome dysbiosis is deeply connected with periodontal disease. Periodontal disease is characterized by gram-negative bacteria overgrowth in between the gums and roots of your teeth (in the pocket). Although some translocation of oral bacteria isn’t a big deal, when you have periodontal disease, you have constant oral microbiota entering the bloodstream.

Interestingly, periodontal disease is a relatively recent human disease. The archaeological record and associated research indicate that preagricultural humans (hunter-gatherers) didn’t get periodontal disease. It wasn’t until the agricultural revolution (10-14 thousand years ago) that archaeologists see the first evidence of periodontal disease (and of dental caries, too!). This is likely due to the dramatic change in diet that accompanied this transition from hunter-gatherer (subsisting on meat, and a variety of plant foods) to agriculture, when diets heavy in grain products became widespread. To learn more about how our oral health and nutrition has changed over evolutionary time click here.
What do you see for the future of Alzheimer’s research?
Haptonstall announced that there has been a sort of “renaissance” going on in Alzheimer’s research. Since the disease has been so difficult to study so far and still such little is known about the cause of the disease, researchers are forced to look outside of their comfort zone. More groups are opting for interdisciplinary models, combining experts from different backgrounds such as neuroscience, immunology, cardiology, dental practitioners, etc., all focused on collaboration.
Circling back to the oral microbiome
The oral microbiome may be the key to early diagnosis and offers a possible starting point for prevention. Healthy mouth, happy body — something we like to say here at Your Autoimmunity Connection. Haptonstall’s current research project is focused on sequencing the oral microbiomes of Alzheimer’s patients in order to develop a blueprint of what the oral microbiome looks like in an individual with Alzheimer’s. Haptonstall concluded by saying “If we can get a good understanding for what the oral microbiome of a healthy individual, pre-disease state, and disease state should all look like, this could revolutionize the way we diagnose, prevent, and treat Alzheimer’s disease — swabbing which could easily take place in any dental office.”
Questions? Please comment below!
References
- S. Dominy, C. Lynch, F. Ermini, M. Benedyk, A. Marczyk, A. Konradi, M. Nguyen, U. Haditsch, D. Raha, C. Griffin, L. J. Holsinger, S. Arastu-Kapur, S. Kaba, A. Lee, M. I. Ryder, B. Potempa, P. Mydel, A. Hellvard, K. Adamowicz, H. Hasturk, G. D. Walker, E. C. Reynolds, R. L. M. Faull, M. A. Curtis, M. Dragunow, J. Potempa, Porphyromonas gingivalis in Alzheimer’s disease brains: Evidence for disease causation and treatment with small-molecule inhibitors. Sci. Adv. 5, eaau3333 (2019).






2 Comments
lordmyrt · May 13, 2020 at 6:31 pm
Here’s an interesting article connecting the oral microbiome with psychiatric diseases: schizophrenia, bipolar and major depression.
It even suggests that schizophrenia may have an autoimmune inflammatory connection!
https://www.psychiatrictimes.com/schizophrenia/whats-your-mouth?elq_mid=11986&elq_cid=1681270
Could a Cure for Alzheimer’s Disease Lie in the Mouth? – DrBonnie360 presents · May 22, 2019 at 8:58 pm
[…] here for more information on current research being done on the oral microbiome and […]